Anterior cruciate ligament (ACL) injuries can be devastating for athletes and active individuals alike. The road from injury to full recovery often involves complex surgical intervention and rigorous rehabilitation. Understanding the intricacies of ACL anatomy, surgical techniques, and post-operative protocols is crucial for patients embarking on this challenging journey. This comprehensive guide explores the latest advancements in ACL treatment, from diagnosis to emerging technologies, providing valuable insights for those facing ACL reconstruction.
ACL anatomy and injury mechanisms
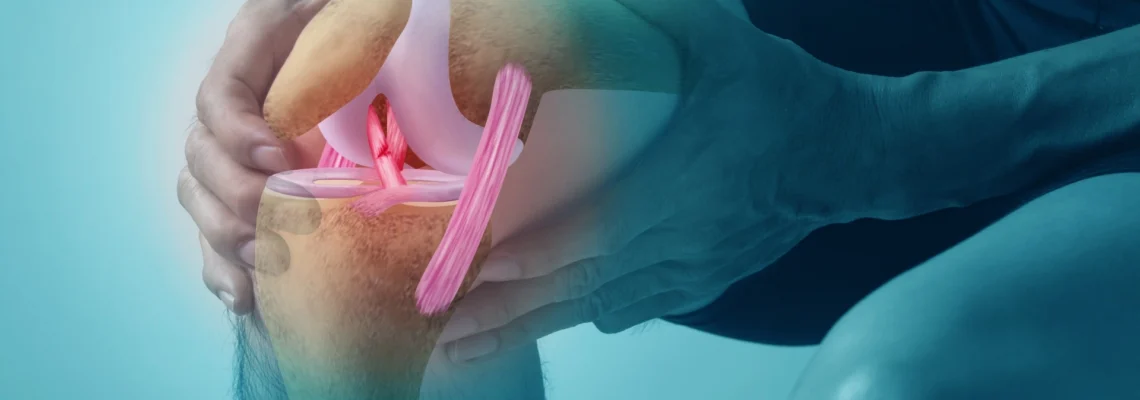
The ACL is a vital stabilizing ligament within the knee joint, connecting the femur to the tibia. Its primary function is to prevent excessive forward movement of the tibia relative to the femur and to limit rotational movements of the knee. ACL injuries typically occur during sudden deceleration, landing, or pivoting movements, often in non-contact situations.
Understanding the anatomy and biomechanics of the ACL is essential for both prevention and treatment. The ligament consists of two distinct bundles: the anteromedial (AM) and posterolateral (PL) bundles. These bundles work synergistically to provide stability throughout the knee's range of motion. When an ACL tear occurs, it can involve one or both bundles, influencing the severity of instability and the approach to surgical reconstruction.
Common injury mechanisms include:
- Sudden changes in direction or cutting maneuvers
- Landing from a jump with the knee extended
- Deceleration combined with a pivot or sidestep
- Direct contact or collision to the knee
Recognizing these mechanisms can help athletes and coaches develop strategies to reduce the risk of ACL injuries through proper training and technique modification. However, when is an ACL operation needed ? This question often arises immediately after injury, and the answer depends on various factors, including the severity of the tear, the patient's activity level, and the presence of associated injuries.
Pre-operative assessment and diagnosis
Accurate diagnosis of an ACL injury is crucial for determining the appropriate treatment plan. A comprehensive pre-operative assessment typically involves a combination of clinical examination, imaging studies, and specialized tests to evaluate knee stability and function.
MRI imaging for ACL tear confirmation
Magnetic Resonance Imaging (MRI) is the gold standard for diagnosing ACL tears. It provides detailed images of soft tissues, allowing surgeons to assess the extent of the ligament damage and identify any associated injuries. MRI has a sensitivity and specificity of over 90% for detecting ACL tears, making it an invaluable tool in the diagnostic process.
Lachman test and pivot shift examination
Clinical examination remains a cornerstone of ACL injury diagnosis. The Lachman test, considered the most sensitive clinical test for ACL insufficiency, involves assessing the anterior translation of the tibia relative to the femur. The pivot shift test evaluates rotational stability and is highly specific for ACL tears when positive.
KT-1000 arthrometer measurements
The KT-1000 arthrometer provides an objective measure of anterior tibial translation. This device quantifies the laxity of the knee joint, offering a numerical value that can be compared to the uninjured knee or used to track progress during rehabilitation. A side-to-side difference of more than 3mm is generally considered indicative of ACL insufficiency.
Concomitant meniscal and cartilage damage evaluation
ACL injuries often occur in conjunction with other knee pathologies. Assessing for meniscal tears and cartilage damage is crucial for comprehensive treatment planning. Arthroscopic evaluation during ACL reconstruction allows for direct visualization and concurrent treatment of these associated injuries, optimizing overall knee function and long-term outcomes.
ACL reconstruction surgical techniques
ACL reconstruction has evolved significantly over the past decades, with surgeons now employing a variety of techniques tailored to individual patient needs. The goal of surgery is to restore knee stability and function, allowing patients to return to their desired level of activity.
Autograft vs. allograft selection criteria
Choosing between autograft (patient's own tissue) and allograft (donor tissue) is a critical decision in ACL reconstruction. Autografts, typically harvested from the patellar tendon or hamstring tendons, offer excellent incorporation and lower risk of graft failure. However, they are associated with donor site morbidity. Allografts eliminate donor site issues but may have a higher risk of failure, particularly in younger, active patients.
The choice between autograft and allograft should be individualized based on patient age, activity level, and surgical history.
Single-bundle vs. Double-Bundle reconstruction
Single-bundle reconstruction has been the traditional approach, replacing the torn ACL with a single graft. Double-bundle reconstruction aims to more closely replicate the native ACL anatomy by reconstructing both the AM and PL bundles. While double-bundle techniques may offer improved rotational stability, their superiority over well-performed single-bundle reconstructions remains debated in the literature.
Anatomic ACL reconstruction approach
Anatomic ACL reconstruction focuses on placing the graft in the native ACL footprint on both the femur and tibia. This approach aims to restore normal knee kinematics more effectively than traditional non-anatomic techniques. Surgeons use various landmarks and imaging techniques to ensure precise tunnel placement, which is critical for graft function and long-term outcomes.
All-inside ACL reconstruction method
The all-inside technique is a minimally invasive approach that uses sockets instead of full tunnels for graft fixation. This method can reduce postoperative pain and accelerate early rehabilitation. It's particularly beneficial for patients with small knee anatomy or those undergoing revision surgery where bone preservation is crucial.
Post-operative rehabilitation protocols
Successful ACL reconstruction is only half the battle; comprehensive rehabilitation is essential for optimal recovery and return to sport. Modern rehabilitation protocols emphasize early motion, progressive strengthening, and functional training tailored to the individual's goals and graft biology.
Early range of motion exercises
Initiating range of motion (ROM) exercises early in the postoperative period is crucial for preventing arthrofibrosis and optimizing graft healing. Patients typically begin passive and active-assisted ROM exercises within the first week post-surgery, gradually progressing to full ROM over the following weeks.
Neuromuscular electrical stimulation (NMES) for quadriceps activation
Quadriceps weakness is a common challenge following ACL reconstruction. NMES has been shown to be effective in facilitating quadriceps activation and strength gains, particularly in the early postoperative period when voluntary muscle contraction may be limited by pain and swelling.
Closed kinetic chain exercises progression
Closed kinetic chain exercises, such as squats and leg presses, are introduced early in rehabilitation to promote functional strength and proprioception. These exercises allow for controlled loading of the graft while minimizing shear forces on the knee joint. Progression from bodyweight exercises to resistance training is guided by functional milestones and graft healing timelines.
Return-to-sport criteria and testing
Determining readiness for return to sport is a critical decision in ACL rehabilitation. A battery of functional tests, including hop tests, agility drills, and sport-specific movements, is used to assess both physical and psychological readiness. Criteria often include achieving >90% strength and functional performance compared to the uninjured limb, as well as demonstrating proper movement patterns and confidence in the reconstructed knee.
| Test | Target Score | Purpose |
|---|---|---|
| Single Leg Hop for Distance | >90% of uninjured limb | Assess power and confidence |
| Y-Balance Test | >90% composite score | Evaluate dynamic balance |
| Isokinetic Strength Testing | >90% quadriceps/hamstring strength ratio | Measure muscle strength symmetry |
Complications and Long-Term outcomes
While ACL reconstruction is generally successful, potential complications and long-term considerations must be addressed. Common early complications include infection, arthrofibrosis, and hardware issues. Long-term concerns include graft failure, contralateral ACL injury, and the development of osteoarthritis.
Recent studies have shown that the risk of graft failure is highest in the first two years post-reconstruction, particularly in young, active patients. Proper rehabilitation and adherence to return-to-sport guidelines are crucial for minimizing this risk. Additionally, attention to neuromuscular control and biomechanics may help reduce the risk of contralateral ACL injury, which occurs in up to 20% of patients within five years of the initial injury.
The long-term impact of ACL reconstruction on knee osteoarthritis remains a subject of ongoing research. While reconstruction may not completely prevent the development of osteoarthritis, it can significantly delay its onset compared to untreated ACL injuries. Patients should be counseled on the importance of maintaining a healthy body weight and engaging in regular, low-impact exercise to promote long-term joint health.
Emerging technologies in ACL treatment
The field of ACL treatment is continually evolving, with new technologies and techniques emerging to improve outcomes and accelerate recovery. These innovations offer promising alternatives to traditional reconstruction methods and may revolutionize ACL injury management in the coming years.
Bridge-enhanced ACL repair (BEAR) technique
The BEAR technique represents a paradigm shift in ACL treatment, aiming to heal the native ligament rather than replace it. This procedure involves placing a special scaffold between the torn ACL ends, which is then injected with the patient's blood to promote healing. Early clinical trials have shown promising results, with patients demonstrating similar outcomes to traditional ACL reconstruction at short-term follow-up.
Platelet-rich plasma (PRP) therapy in ACL recovery
PRP therapy has gained popularity in sports medicine for its potential to enhance healing and reduce recovery time. In ACL reconstruction, PRP may be used to augment graft healing and improve outcomes. While research is ongoing, some studies have shown improved graft maturation and reduced pain when PRP is applied during surgery or in the early postoperative period.
Computer-assisted surgery for ACL reconstruction
Computer-assisted navigation systems are being increasingly utilized in ACL reconstruction to improve the precision of tunnel placement and graft positioning. These technologies provide real-time feedback to surgeons, potentially leading to more anatomically accurate reconstructions and improved functional outcomes. As these systems become more refined and user-friendly, they may become standard tools in ACL surgery.
The journey from ACL injury to full recovery is complex and demanding, requiring a multidisciplinary approach and patient dedication. Understanding the intricacies of ACL anatomy, surgical techniques, and rehabilitation protocols is crucial for optimizing outcomes. As emerging technologies continue to advance the field, patients can look forward to increasingly personalized and effective treatment options. With proper care and commitment to rehabilitation, most individuals can expect to return to their desired level of activity following ACL reconstruction.